The Steroidogenic Pathways – The Hormone Highway Begins Here
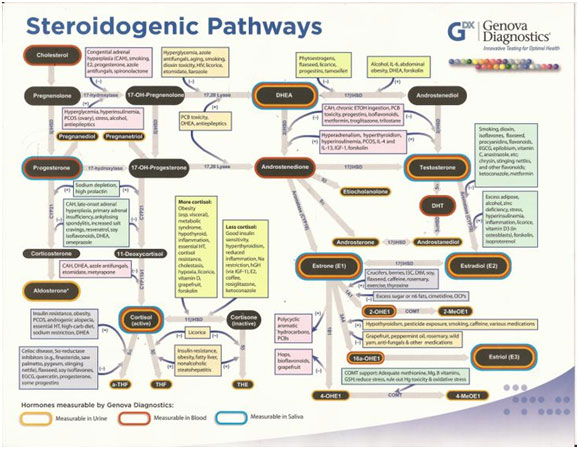
Hormones do not work alone. Every estrogen surge, testosterone boost, or cortisol spike starts with a single master molecule: cholesterol. (1)
That’s right—the much-maligned fat molecule is actually the raw material for all sex hormones.
When cholesterol levels drop below 140 mg/dL, the body simply can’t make enough of its key hormones. This includes estrogen, progesterone, testosterone, DHEA, and cortisol—all of which rely on one critical intermediate: pregnenolone
🔄 From Cholesterol to Hormonal Harmony
- Cholesterol → Pregnenolone
- Pregnenolone branches into:
- DHEA
- Progesterone
- Testosterone
- Estrogen
- Cortisol
🧠 Why Pregnenolone Matters
Pregnenolone isn’t just a hormone precursor—it’s a hormone powerhouse on its own. It:
- Buffers cortisol, enhancing your stress resilience
- Reduces inflammation and pain
- Boosts memory, focus, and nerve transmission
- Improves mood, learning, and sleep
- Supports nerve repair
⏳ The Aging Effect
As we age, pregnenolone levels naturally decline—by as much as 65% by age 75 compared to age 35. Low levels are linked to:
- Arthritis
- Insomnia
- Brain fog and poor memory
- Fatigue and depression
- Reduced ability to handle stress
Common causes of low pregnenolone include:
- Low cholesterol (<140 mg/dL)
- Hypothyroidism
- High intake of trans or saturated fats
- Certain tumors
⚠️ Too Much of a Good Thing?
While deficiency is more common, excessive pregnenolone can cause:
- Fluid retention
- Drowsiness
- Irritability
- Headaches
- Palpitations
- Insomnia
🎯 Optimal Levels
The ideal blood level of pregnenolone:
- 90-110 ng/dL (2)
DHEA-The Master Hormone Precursor:
Dehydroepiandrosterone (DHEA) is produced in the adrenal glands, brain, and skin, where it serves as a vital precursor to estrogen and testosterone in both men and women. Often called the “mother of all steroid hormones,” DHEA influences dozens of biological systems.
🔻 Natural Decline with Age
Like other hormones, DHEA production declines over time. By age 70, most people produce only 10–20% of the amount present at age 20.
🧬 What DHEA Does
DHEA plays a wide-ranging role in restoring and protecting health:
- Improves mood and well-being
- Supports immune function and tissue repair
- Reduces allergic response and systemic inflammation
- Enhances brain function and memory
- Increases lean body mass and reduces body fat
- Lowers triglycerides and cardiovascular risk
- Improves insulin sensitivity and helps prevent type 2 diabetes
- Acts as a natural antioxidant
- May slow biological aging (shown in animal models)
- Supports bone health, reduces osteoporosis and atherosclerosis risk
- Improves sleep and reduces depressive symptoms
⚖️ What Causes DHEA Deficiency?
- Aging
- Menopause
- Chronic stress
- Tobacco use
⚠️ Signs of Excess DHEA
While deficiency is common, excessive DHEA supplementation may lead to:
- Fatigue
- Irritability
- Insomnia
- Mood swings
- Weight gain
- Sugar cravings
- Acne and hirsutism (excess facial or body hair growth)
🎯 Optimal Blood Levels (3)
- Men: 500–600 ng/dL
- Women: 200–250 ng/dL
Side effects associated with excess DHEA include acne and hirsutism.

Hormonal Regulators — DHT, Cortisol, and Insulin
🔹 Dihydrotestosterone (DHT): The Powerful Derivative of Testosterone
DHT (Dihydrotestosterone) typically accounts for 10–15% of total testosterone and is a potent androgen that significantly influences hair, skin, sexual function, and prostate health.
✅ Benefits of DHT
- Enhances libido
- Increases energy and motivation
⚠️ Risks of Excess DHT
- Accelerated hair loss (especially male-pattern baldness)
- Prostate enlargement (BPH)
- Acne
- Reduced sperm production
- Erythrocytosis (elevated red blood cells)
- Gynecomastia
- Sleep apnea
- Fetal virilization (in utero exposure)
🎯 Optimal DHT Levels
- 100–500 ng/dL
🩺 DHT Management Options
- Scutellaria baicalensis “Chinese Skullcap”-Dose 1-2 gm/d
- DIM 3-Dose 1-3 gm/d (with Bioperine 2.5 mg)
- Vitamin D3-Tirate to serum level 50-80 ng/dL
- Probiotic + Colostrum
- Megaspore 1/d
- Colostrum 10-30 gm/d
- Iodine-150-225 mcg/d
- Pregnenolone-25-30 mg 2x/d
- Zinc-30 mg 2x/d
- Mucuna pruriens-250-1000 mg/d
- UltraClear Sustain (BCAA’s)-1 scoop in 8 oz liquid daily
Note: We do not recommend 5 alpha reductase inhibitors, finasterinde or dutasteride due to post finasteride syndrome. (Can we hyperlink this to the article on website?)
🔸 Cortisol: The Stress Hormone with Dual Roles
Cortisol, produced by the adrenal glands, is one of the few hormones that increases with age (the other is insulin). It plays a crucial role in energy balance, stress response, immune modulation, and metabolic control.
🧠 Normal Stress Response
- Cortisol rises during stress and should return to baseline when stress is resolved.
⚠️ Chronic Elevation (Adrenal Dysregulation)
When stress becomes chronic or unmanaged, cortisol remains elevated, contributing to:
- Irritability and mood swings
- Sugar cravings
- Chronic fatigue and muscle weakness
- Night sweats and insomnia
- Abdominal fat accumulation
- High blood pressure, lipids, and blood sugar
- Immune suppression and frequent infections
- Impaired thyroid function and thin skin.
🔁 Hormonal Imbalance Triggered by Cortisol
- Decreases progesterone production
- Increases thyroid hormone binding, reducing its activity
🎯 Key Functions of Cortisol
- Regulates blood sugar and energy
- Supports immune modulation and protein synthesis
- Influences mood, sleep, and bone turnover
🧪 Preferred Testing
- 4-point salivary cortisol panel (morning, noon, afternoon, night)
- Also test salivary DHEA-S, progesterone, estrogen, testosterone
- Pair with capillary blood glucose readings for adrenal/metabolic mapping
✅ Strategies to Normalize Cortisol
- DHEA replacement (if low)
- Adaptogenic herbs (e.g., Rhodiola, Ashwagandha, Licorice root extract)
- Anti-inflammatory diet
- Key nutrients:
- B-complex, vitamin C
- Magnesium, calcium, zinc, selenium, copper, manganese
- Omega-3 fatty acids, phosphatidylserine
- Multi-glandular adrenal formulas
- Lifestyle: Stress reduction techniques (mindfulness, breathwork, restorative sleep).
🔻 Insulin: The Blood Sugar Regulator & Inflammatory Trigger
Insulin is secreted by the pancreas and plays a vital role in:
- Converting glucose into energy (or fat if unused)
- Promoting muscle development
- Preventing blood sugar spikes
- Counterbalancing cortisol and adrenaline
✅ Benefits
- Supports glucose uptake
- Lowers blood sugar
- In men: Testosterone enhances insulin function
- In women: Estrogen promotes similar metabolic effects
⚠️ Signs of Insulin Deficiency
- Bone loss
- Depression
- Fatigue
- Insomnia
Caused by:
- Low-carb diets
- Over-exercising
- Caloric malnutrition
⚠️ Risks of Excess Insulin
- Acne, asthma
- Mood swings, sugar cravings
- Hypertension, high cholesterol
- GERD and cardiovascular disease
- Breast and colon cancer
- Decreased testosterone in men
- Estrogen/testosterone imbalance in women
- Insomnia and fluid retention
Insulin levels often rise for years before glucose becomes abnormal, making insulin a critical early biomarker for metabolic dysfunction.
🧪 Root Causes of Insulin Resistance or Hyperinsulinemia
- High-carbohydrate diets
- Sugared beverages and snacks
- Low-fat/high-sugar diets
- Caffeine or alcohol overuse
- Hyperthyroidism
- Estrogen or testosterone imbalances
- Sedentary lifestyle
- Smoking
- Medications (e.g., beta-blockers, steroids, antidepressants, diuretics)
✅ Nutritional & Supplement Strategies for Improving Insulin Sensitivity
- Anti-inflammatory diet
- Soluble fiber (e.g., oat bran, psyllium)
- Omega-3s (EPA/DHA)
- Chromium
- Alpha-lipoic acid
- Vanadium
- Antioxidants: Vitamins A, C, E + Selenium
- CoQ10
- Cinnamon
- Green tea & green coffee extract
- Maitake mushroom extract
🎯 Optimal Ranges
- Serum insulin: 5–10 μU/mL
- Glucose-to-insulin ratio: ~10:1
Melatonin & Growth Hormone – The Sleep and Vitality Regulators
🌙 Melatonin: The Body’s Circadian Timekeeper and Cellular Protector
Melatonin is primarily produced by the pineal gland and secondarily by the retina, gastrointestinal (GI) tract, and white blood cells. It plays a key role in regulating the circadian rhythm, helping the body fall asleep, stay asleep, and synchronize biological functions with light-dark cycles.
✅ Melatonin’s Functions and Benefits
- Promotes restful sleep and resets circadian rhythm
- Helpful for insomnia and jet lag
- Synthesized from tryptophan (requires B vitamins)
- Potent antioxidant that scavenges free radicals
- Lowers cortisol, supporting adrenal recovery
- Enhances immune function
- Blocks estrogen receptor binding (may reduce estrogen dominance)
- May have anti-cancer and anti-aging properties
- Improves mood, sleep quality, and stress response
- Stimulates growth hormone and parathyroid hormone production
- Reduces:
- Blood pressure
- Migraine and cluster headache frequency
- Nocturia (nighttime urination)
- Inflammatory burden
⚠️ Factors That Deplete Melatonin
- Alcohol, caffeine, and tobacco use
- Certain medications (e.g., beta blockers, NSAIDs)
- EMF (electromagnetic field) exposure
- Shift work and artificial light at night
⚠️ Sources of Excess or Sensitivity
Some foods and herbs naturally boost melatonin:
- Bananas, cherries, oats, rice, corn, tomatoes, ginger, walnuts
- St. John’s Wort
- Over-exercising or over-supplementing
🎯 Melatonin Supplementation
- Most effective form: Compounded micronized melatonin
- Dose range: 3 to 30 mg, titrated to response
- Best taken ~1 hour before bedtime
🔍 Response Variability
- ~10% of patients may not respond
- ~1% may experience paradoxical stimulation
- Minimal effect in chronic sleeping pill users
- Rare side effects: Grogginess, and hair repigmentation (darkening)
💪 Growth Hormone (GH): The Regenerator of Youthful Physiology
Growth hormone declines by up to 75% from early adulthood to midlife, triggering a cascade of aging-related effects:
- Loss of lean muscle mass
- Accumulation of body fat
- Thinning skin
- Decreased vitality and mobility
✅ Benefits of GH Replacement Therapy
- Increases basal metabolic rate by 6–11% within 6 months
- Enhances lean body mass and reduces fat
- Improves sexual function and performance
- Promotes hair regrowth and skin thickness
- Supports cardiovascular health by:
- Reducing triglycerides, total cholesterol, and LDL
- Preventing carotid artery thickening
- Improving cerebral blood flow and cardiac output
- Improves lung function and exercise tolerance
- Enhances sleep quality—including REM and slow-wave sleep
- Boosts energy, mood, emotional resilience, and pain tolerance
⚠️ GH Deficiency Is Linked To
- Increased risk of cardiovascular disease and atherosclerosis
- Decreased bone mineral density and osteoporosis
- Declines in physical, emotional, and sexual well-being
- Doubled risk of certain cancers when GH levels are abnormally low
🦴 Bone Density Improvements with GH Therapy
- GH increases bone mineral density (BMD) by 6–15%
- Best results occur in women receiving estrogen plus bisphosphonate therapy (e.g., Fosamax, Actonel)
Positive Effects and Considerations of Growth Hormone Replacement
– Positive effects of growth hormone replacement is not typically evident for at least 6 months.
– Side effects of growth hormone (dose-dependent) may include edema, arthralgias, myalgias (notably carpal tunnel syndrome), and short-term glucose intolerance.
– No long-term changes in fasting blood sugar or insulin levels have been observed in studies spanning 7 and 10 years. A transient increase in insulin resistance may occur within 1-6 weeks, which can persist for up to 18 months. However, there is no evidence of an increased incidence of diabetes compared to the general population (12).
– There is no evidence that growth hormone replacement increases cancer risk.
Growth hormone levels are monitored via IGF-1 levels. Optimal IGF-1 levels for adults are typically between 300 and 350 ng/mL. Side effects are more likely when levels exceed 380 ng/mL.
– The standard dose of growth hormone is 0.1 mg/day administered subcutaneously. The dose may be titrated upward to 0.2, 0.4, or 0.8 mg/day, with a maximum of 1.2 mg/day.
References
– Tsujimura, A., et al. “Treatment with human chorionic gonadotropin for PADAM.” *Aging Male*, 2005 Sept-Dec; 8(3-4):175-179.
– Hanaway, Patrick. *Estrogen Metabolism Hormone Essentials: Presentation* at A4M Lecture Series, Las Vegas, NV, December 10, 2010.
– Hertoghe, The Hormone Handbook, 2006, International Medical Publications, UK, p. 221.
– Bassil et al. “The benefits of testosterone replacement therapy: A review.” *Therapeutics and Clinical Risk Management*, 2009; 5:427-448.
– [Wellness Hormone Balance](http://www.wellnesshormonebalance.org/files/)
– [BodyLogicMD Testosterone Levels](http://www.bodylogicmd.com/for-men/testosterone-levels)
Other Hormones Symptoms
| Growth Hormone | DHEA |
|---|---|
| Thinning Hair | Dry Hair |
| Sagging Cheeks | Dry Skin and Eyes |
| Receding Gums | Flabby Muscles |
| Flabby Abdomen | Flabby Abdomen |
| Slack Muscles | Little Hair Under Arms |
| Skin Thin and Dry | Scant Pubic Hair |
| Poor Recovery from Physical Activity | Scant Fatty Tissue in Pubic Area |
| Profound Fatigue | Noise Intolerance |
| Isolates Self (“I hate everyone”) | Poor Libido |
| Overwhelming Anxiety and Worry | Poor Sexual Scent |
Melatonin & Insulin
| Melatonin | Insulin |
|---|---|
| Aging Faster Than Peers | Craves Sweets |
| Difficulty Falling Asleep | Always Thirsty |
| Difficulty Staying Asleep | Urinates Frequently |
| Mind Races at Night | Slow Healer |
| Difficulty Recovering From Long Trips | Skinny Stomach and Buttocks |
| Night Shift or Swing Shift Worker | |
| Lives Out of “Sync” with World | |
| Often Jet Lagged | |
| Often Takes Sleeping Pills | |
| Tired Upon Rising |
